The vestibular system plays a critical role in maintaining the sense of balance and equilibrium. The structures within the inner ear are considered part of the peripheral vestibular system and are full of motion sensors that detect motion and send that information to the brain. The brain interprets the information and determines the position of the head in space. This blog will discuss two different pathologies that can occur in the inner ear that can cause significant dizziness and how Physical Therapists can be equipped to treat them.
Benign Paroxysmal Positional Vertigo
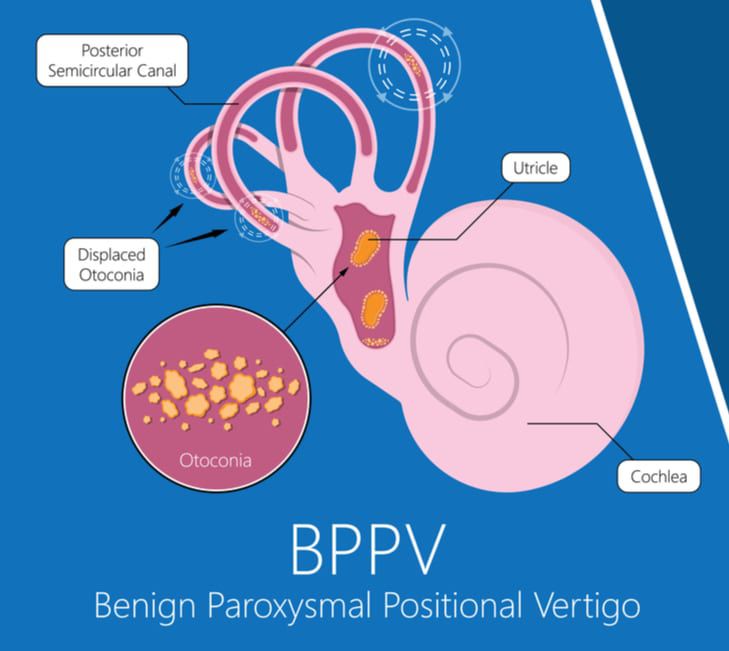
BPPV is the most common disorder of the peripheral vestibular system. It happens when the otoconia, that are usually in the utricle, are forcefully displaced into one of the three semicircular canals confusing the motion sensors in the ear leading to extreme and sudden vertigo. BBPV often occurs after a traumatic event, but can also happen idiopathically or with specific head movements
“Every time I roll over in bed, I feel like the room immediately begins to spin”
*Note that these patients will use the term “spinning” or “spin” to describe their dizziness.
Can Physical Therapists Treat BPPV?
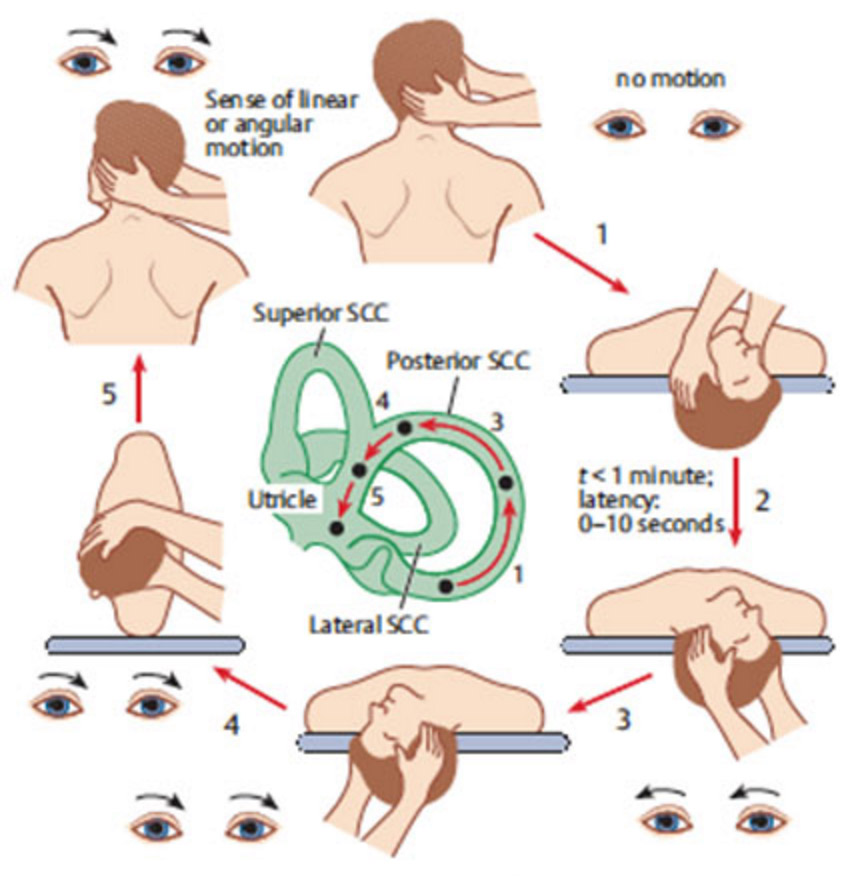
Yes! A Physical Therapist might ask a few questions and conduct a few tests to establish BPPV as a diagnosis. For treatment, the therapist will guide you through a series of positions to allow the displaced otoconia to return to their correct position within the inner ear. It is usually a relatively easy and quick fix if the positional maneuver is done correctly. Only two or three additional visits may be required to ensure that all otoconia are back where they belong.
Vestibular Hypofunction
Vestibular hypofunction encompasses peripheral vestibular disorders such as neuritis, and labyrinthitis and are usually caused by infections to the inner ear or traumatic events. In this case, dizziness is usually exacerbated with head movement. The main culprit is often a malfunctioning vestibulo-ocular reflex (VOR). The VOR is crucial in stabilizing the eyes while the head is moving, and can be problematic if it is impaired. If the eyes cannot keep up with the head as it moves, it can lead to significant dizziness, and can have a detrimental effect on daily activities such as driving, reading, crossing a busy street, etc.
“I get off balance and very dizzy every time I turn to the left, so I avoid doing so”
*Note these patients will not use the word “spinning” or “spin” to describe their dizziness.
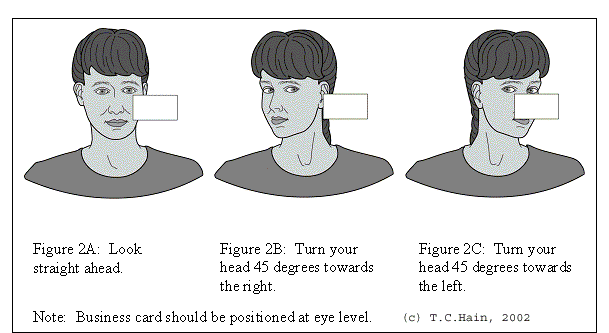
Can Physical Therapists Treat Vestibular Hypofunction Too?
For the most part, yes. For treatment, the therapist will walk the patient through a series of exercises aimed at stabilizing their gaze. The goal of the exercises is to essentially re-train the brain to not get dizzy with head movements. Treatment for a vestibular hypofunction is usually longer (6-12 weeks), as it takes time for the patient to progress from simple to more complex gaze stabilization exercises.
Final Thoughts
Dizziness can be truly debilitating and affect virtually every facet of life. It is not well known, even to fellow health care providers, that physical therapy can effectively treat vestibular disorders, yet it is well within the Physical Therapy scope of practice.
If you’re suffering from dizziness, contact REHAB AT WORK today to see if physical therapy and rehabilitation might be a good option for you!

Article by Rebecca White, PT, DPT
References:
- Aguilera M, Campbell D, Gallegos D. Vestibular Rehab to the Rescue. Rehab Management: The Interdisciplinary Journal of Rehabilitation. 2020; 33(2): 18-21.
- Arnold SA, Stewart AM, Moor HM, Karl RC, Reneker JC. The Effectiveness of Vestibular Rehabilitation Interventions in Treating Unilateral Peripheral Vestibular Disorders: A Systematic Review. Physiotherapy Research International. 2017; 22(3) n/a-N PAG. doi: 10.1002/pri. 1635
- Farrell L. Peripheral Versus Central Disorders: Fact sheet. Vestibular Rehabilitation Special Interest Group of the Academy of Neurologic Physical Therapy.
- Hall CD, Herdman SJ, Whitney SL, et al. Vestibular Rehabilitation for Peripheral Vestibular Hypofunction: An Evidence-Based Clinical Practice Guideline: FROM THE AMERICAN PHYSICAL THERAPY ASSOCIATION NEUROLOGY SECTION. J Neurol Phys Ther. 2016;40(2):124-155. doi:10.1097/NPT.0000000000000120




